Antimicrobial Release fromResorbable Temperature-Responsive Hydrogels is Effective at Controlling Infection
Authors: McLemore R, Overstreet D, McLaren A, Jarbo K, DovigiA, VernonB. Banner Good Samaritan Medical Center, Phoenix AZ and Arizona State University, Tempe AZ
Title: Antimicrobial Release from Resorbable Temperature-Responsive Hydrogels is Effective at Controlling Infection
Background: Previously, we have reported on the controlled release properties of a novel temperature-responsive hydrogel based on copolymers of N-isopropylacrylamide and Jeffamine® M-1000 acrylamide (PNDJ hydrogel).that is viscous, provides sustained antimicrobial release over 7 days in vitro, and degrades in 9-40 days. Because the delivery and degradation time is short, it is unclear if antimicrobial release from these materials will be long enough duration to be effective fort controlling orthopaedic infections.
Hypothesis/Purpose: Is release of antimicrobials from copolymers of NIPAAm and Jeffamine (PNDJ hydrogel) effective at controlling infection?
Methods: The Nelson radial defect infection model was used to establish infection in NZW rabbits infections were confirmed grossly, histologically and on culture, At 3 weeks the infections were debrided and implanted with a metal implant, and randomly selected for local delivery with 5wt% gentamicin PNDJ hydrogel or saline control. 9 animals received gentamicin PNDJ hydrogel and 9 received no local delivery. Systemic antimicrobials were not used in either group. Open biopsy culture and harvesting of the infection site for histological analysis was performed 4 weeks post debridement.
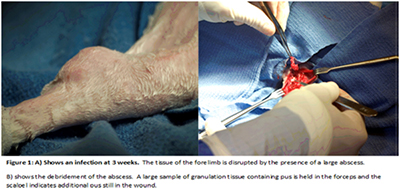
Results: 18/18 animals were successfully infected. Abscess formation (Fig1), positive histology and cultures positive for the inoculum Staphylococcus Aureus occurred in all.. Animals that received local gentamicin delivery from PNDJ hydrogel had a lower rate of continuation of infection after debridement than animals without local antimicrobial delivery (p<0.001). Gross inspection showed close tissue apposition to the implant in all local delivery animals. There was no evidence of a local tissue response to the gel or the gel remaining in the local depot sites.
Discussion: PNDJ hydrogels were well-tolerated following debridement for an active infection. Sufficient antimicrobial was delivered to decrease the rate of infection continuing after debridement. These data are consistent with the goal of using PNDJ hydrogel for antimicrobial delivery in the management of orthopedic infections when antimicrobial loaded bone cement is not used.
Conclusion: Antimicrobial delivery from PNDJ hydrogel is effective in the management of orthopaedic infections.